10 Tips for Preventing Tick-borne Diseases This Summer 07/07/2013
Posted by thetickthatbitme in Prevention, TBID Facts.Tags: armor, Borrelia, golf, hiking, Lyme Disease, prevention, tick, tick bite, Tick-borne disease
6 comments
It’s officially questing season for ticks. Billions of blood-loving arachnids are looking for their next meal, and it could be you. This wouldn’t be such a problem if ticks didn’t carry so many life-disrupting (and sometimes fatal) diseases. Here are 10 tips for avoiding the bite and its potential consequences.
1. Don your armor. Ticks attach to your skin. The best way to prevent this is to keep skin covered and to wear clothing that is treated with a tick repellent (like permethrin or cedar oil). Long pants are a must; tuck them into your socks or boots. (I know it looks stupid, but if enough people do it, it will become cool–I promise. It’ll be like wearing UGG boots with a miniskirt.) I’d also recommend long sleeves and a hat (better for ticks to end up on your hat than on your scalp). Wearing light colored clothing makes it easier for you to spot ticks on you.

Image via http://hovermansion.wordpress.com
2. Avoid high-risk areas. Yes, this seems like a no-brainer, but many people mistakenly believe that you have to be hiking to pick up ticks. In order to avoid ticks, you have to understand that ticks can be carried by almost any mammal or bird—not just deer and mice. If you’re in a place where wildlife is found (even if that place is your backyard), there’s a chance that ticks will find you. In particular, you should avoid wooded areas, tall grasses, leaf piles, cabins that may be infested with mice or rats, and picnic areas (a.k.a. tick restaurants). Also, keep in mind that ticks are found on domestic animals, including dogs, cats, cattle, and horses (don’t even get me started on petting zoos—oh, hello Q fever…)
3. If you must enter the danger zone, use common sense and be vigilant. When hiking, stay in the middle of trails and keep your distance from wild animals—no feeding the squirrels, etc. If you’re an avid golfer, don’t go trudging into the rough to retrieve your ball. Your score may suffer, but your immune system will thank you. Don’t believe me? Read this.
4. After outdoor time, do a proper debriefing (pun intended). When you come back indoors, before you hug the kids, post pics to Instagram, do the dishes, WHATEVER, remove your armor and toss it in the dryer. (Yes, before you wash it.) Experts used to say that an hour on high heat was necessary to kill ticks on clothing, but it may take as little as five minutes on low. See this article about Jacqueline Flynn, a high school student who researched tick-cide by dryer. Once your armor is in the dryer, it’s shower time for you—but first, you need to do a naked tick check. (Enlist the help of a spouse or family member, and don’t be embarrassed. Monkeys do this all the time.) Remember, nymphal ticks can be as small as a poppy seed, so you need to look carefully. Don’t forget to check the scalp, armpits, backs of knees, and groin area.
5. Preserve the evidence. If you find any ticks, don’t squash them, burn them, or flush them down the toilet. If a tick is on you, it might have bitten you, and you need to have it identified and tested to see what you may be dealing with. If a tick is attached to you, remove it gently with tweezers and put it in a closed container like a prescription bottle. Then call your doctor’s office and tell them you have a tick you’d like identified and tested.
6. Protect the pack. Your dog or cat is vulnerable to tick exposure as well, and ticks can easily hitch a ride into your house on your pet. Treat your pet with a vet-recommended tick repellant and do a tick check every time he/she comes in from outside. Keep your pet out of danger zones (including woods, leaf piles, and dog parks) during the summer months (tick questing season). Also, it’s strongly recommended that pets have their own bed instead of sharing yours.
7. Take control of your yard. Regularly dispose of fallen leaves, and mow your lawn short to decrease the likelihood that ticks will hang out there. Dispose of temptations for rats, mice, other rodents, and deer (fallen fruit, dog droppings, trash, etc.). Move wood piles (a.k.a. rat habitats) away from your house, and make sure all outbuildings (sheds, garages) are free of mice, rats, and other critters. You may also want to try spraying your yard for ticks—you can go the chemical or natural route, depending on what you’re comfortable with. Lastly, remember that birds carry ticks, too, so don’t attract them to your yard with bird feeders and bird baths (a.k.a. disease breeding pools). If you want to bird-watch, invest in a good pair of binoculars.
8. Take control of your house. Mandate that all humans and animals entering your home following outdoor activities undergo proper tick-checking procedures. Educate family members about the danger zones and how to spot ticks. To avoid your home becoming a danger zone, make sure there are no unwanted houseguests in the attic, crawl space, or walls (including mice, squirrels, raccoons, feral cats, and birds).
9. Know what you’re looking for. There are many different types of ticks—deer ticks, dog ticks, lonestar ticks, soft-bodied ticks. Depending on where you live, you may have a few or all of these in your neighborhood. Technically, ticks are spiders—they have eight legs—but they look different from spiders in that their bodies are larger in proportion to their legs. If you see something on your body that looks like a tick, don’t waste time trying to identify whether or not it’s a tick—get your tweezers and remove it ASAP, get it into a container, and then worry about what kind it is. See this post for some up-close tick pics.
10. Know who to call. Make sure that your primary care physician and/or infectious disease specialist is on-board with your disease prevention plan. Ask about tick testing. Do you need an appointment to drop off a tick for testing? Can the lab your doctor uses provide containers for tick collection? Is your doctor willing to prophylax you (prescribe a short course of antibiotics within 48 hours) if you get a tick bite? If your doctor is not on board, you can appeal to him or her by sharing the research, or you can start shopping for a new doctor.
Related articles
- Six Tick Misconceptions
- What Is Prophylaxis, and Does It Work on Tick Bites?
- Tick Season in Portugal….are you aware of the problems associated with ticks? (silvercoastangelicdogs.wordpress.com)
- Tick Safety Tips for Kids at Summer Camp (nlm.nih.gov)
9 things you need to know about Borrelia miyamotoi 02/18/2013
Posted by thetickthatbitme in Diagnosis, Media, TBID Facts.Tags: Borrelia, Borrelia hermsii, Borrelia miyamotoi, health, Lyme Disease, medicine, New England Journal of Medicine, Relapsing Fever, tick bite, tick-borne relapsing fever
4 comments
Several months ago, when the patient support group that I attend first began discussing Borrelia miyamotoi, a Google search (or Bing…whatever…) for those two odd words yeilded very little. Now, after the publishing of a few key papers in the New England Journal of Medicine, every major news outlet seems to be aware of this “new” Borrelia.
From a scientific perspective, Borrelia miyamotoi is interesting because it challenges a dichotomy that was established by researchers of tick-borne infectious diseases. When I first started reading about the Borrelia genus, I learned that Borrelia species could be sorted into two major categories: the Lyme disease-like group and the relapsing fever group. That is, Borrelia species like B. burgdorferi, B. afzelli, and B. garinii–which are genetically more similar, are carried by hard-bodied ticks, and cause the same pattern of symptoms (rash, joint pain, fatigue–were put in one group. Other species, like B. hermsii and B. parkeri–which differ genetically from these Lyme-like bacteria, are carried by soft-bodied ticks, and all cause relapsing fever symptoms–were put in the other group. One group for Lyme-like illness. Another group for relapsing fever-like illness. One group for hard-bodied ticks. Another group for soft-bodied ticks. The dichotomy is so clear that the ticks are sometimes referred to as “Lyme disease ticks” and “relapsing fever ticks.”
The funny thing about dichotomies is that they only create the illusion of two distinct categories. The reality is far more messy and characterized by shades of grey. Enter Borrelia miyamotoi. According to its genetics, it should go in the relapsing fever group, but it’s transmitted by the same hard-bodied ticks that carry Lyme disease. According to its symptoms, it falls somewhere in the middle. About 10% of people get a rash, like with Lyme disease, while others don’t. Some people get relapsing fevers, while others don’t. It’s all so very confusing!

A Borrelia family tree (technically called a phylogenetic tree) highlighting strains of B. miyamotoi. Note the groupings of the other Borrelia. Via Platonov AE, Karan LS, Kolyasnikova NM, Makhneva NA, Toporkova MG, et al. (2011) Humans infected with relapsing fever spirochete Borrelia miyamotoi, Russia. Emerg Infect Dis 17: 1816–1823.
As usual, both the researchers and the news media seem to be trying to downplay this. Some are unwittingly obscuring the issue altogether. “Paging Dr. House: There [sic] a new tick-transmitted spirochete in town…” writes Melissa Healey of the L.A. Times. “The New England Journal of Medicine on Thursday published two reports documenting its arrival on U.S. shores.” As if the bacteria hopped on a boat from Russia, and that’s how it got here! Forget the strong possibility that it was here all along and our scientists just failed to detect it. Forget the possibility that the countless numbers of people who tested negative for Lyme disease and were denied treatment could in fact have this similar infection.
Dr. Peter Krause, lead author on the NEJM study, says (in a video for Yale News) he doesn’t think people should panic about Borrelia miyamotoi. At the same time, he admits that this is an infection that is affecting people in both the eastern and western United States–not to mention people in Europe and Asia. “We expect this disease to be found everywhere the deer tick is found,” he states. So don’t panic, but it’s everywhere.
Okay, so Dr. Krause is right when he says people shouldn’t panic, but that doesn’t mean that we shouldn’t learn more about this new–or not so new, as the case may be–infection, especially since many of us could have it right now. Here are nine things I think you should know about Borrelia miyamotoi.
1. Symptoms: Borrelia miyamotoi causes symptoms of tick-borne relapsing fever (TBRF), an illness often misdiagnosed as Lyme disease, or not diagnosed at all. Tick-borne relapsing fever, when left untreated, has some symptom overlap with Lyme: arthralgias, myalgias, chronic fatigue, and cognitive problems; however, it differs from Lyme disease in that most patients with TBRF get repeated episodes of fever, and they don’t get erythema chronicum migrans (EM), the “classic Lyme” bull’s-eye rash. We can guess that the long-term effects of B. miyamotoi infection are similar to those of other Borrelia infections, even if researchers are reluctant to admit it. Dr. Peter Krause, one of the authors of the study published in the January 17 issue of the New England Journal of Medicine, told the L.A. Times: “This is a very new disease, but none of the patients have had this long-term [neurological] trouble or other long-term symptoms,[…] it’s possible that we just haven’t seen it yet.” Long-term neurological problems from a disease that most doctors didn’t know existed until a few months ago? I’d say it’s very possible.
2. Transmission: Borrelia miyamotoi is transmitted to humans from the bites of hard-bodied ticks. Examples of these ticks include Ixodes scapularis (deer tick), Ixodes pacificus (western blacklegged tick), Ixodes ricinus (castor bean tick), and Ixodes persulcatus (taiga tick). (The first two tick species listed are common in North America, and the second two are found in Europe and Asia.)
3. Why you’re just hearing about it now: The B. miyamotoi bacterium was discovered in ticks and mice in Japan back in 1995. (It’s named after Japanese entomologist Kenji Miyamoto, who first isolated the bacterium.) In 2001, Dr. Durland Fish discovered B. miyamotoi in ticks in Connecticut, but according to a 2011 New York Times report, he “was repeatedly refused a study grant [from NIH] until the Russians proved it caused illness.” In 2011, Russian scientists, in collaboration with the Yale team that included Krause and Fish, published research that showed that B. miyamotoi infects humans. The patients in the 2011 study were in Russia, so B. miyamotoi didn’t really come on the radar for U.S. doctors until January 2013, when a study on U.S. patients was published by Krause and colleagues in the New England Journal of Medicine.
4. Testing: To my knowledge, there is currently no commercially-available test for B. miyamotoi, be it PCR, IFA, or Western Blot. B. miyamotoi has been detected using assays (tests) that were developed by university researchers in order to study the bacterium. That means, unless your doctor is at Yale or another large institution, it’s not likely that he or she has access to a test for B. miyamotoi. So if you suspect you may be infected, what can you do? That brings me to my next point.
5. People with B. miyamotoi infection are likely to test negative for B. burgdorferi (Lyme disease), unless they also happen to be infected with B. burgdorferi. Doctors who are only screening patients for Lyme disease are not going to catch all of the other Borrelia infections, like B. miyamotoi.
6. Genetically, B. miyamotoi is more similar to other bacteria that cause TBRF, like Borrelia hermsii. Therefore, people with B. miyamotoi infection may test positive for B. hermsii, another relapsing fever spirochete.
7. As with any infection, B. miyamotoi infection can be more serious in the elderly and in patients with compromised immune systems. If you or a family member is denied treatment, especially in the case of severe or life-threatening symptoms (like high fever), my advice would be to go to a tertiary care center (like a university hospital) and ask to be tested for B. miyamotoi. At the very least, doctors at a research hospital should be able to do a blood smear to look for spirochetes (Borrelia). PCR and antibody tests may also be available.
8.Treatment: B. miyamotoi probably responds in a similar way to antibiotics as other Borrelia like B. hermsii and B. burgdorferi. Researchers claim that it can be treated with a few weeks of oral antibiotics, but that is probably only for mild, acute cases. My guess (as a non-medical-professional) is that B. miyamotoi is just as resilient as its Borrelia cousins and requires 4-6 weeks of daily IV antibiotics. If you’re new to this blog, you might be interested in reading about my experience being treated with IV antibiotics for B. hermsii (relapsing fever).
9. Recommended reading: To learn more about B. miyamotoi, check out the new fact sheet, which includes links to peer-reviewed studies.
Related articles
Parasites in the blood supply, and 7 other things you need to know about Babesia 04/27/2012
Posted by thetickthatbitme in TBI Facts.Tags: Babesia, Blood donation, Blood transfusion, health, Malaria, medicine, Mepron, parasite, pregnancy, Rhode Island Blood Center, tick bite
6 comments
The fact sheet for Babesia is up today. Here are a few (disturbing) highlights:
1. Babesia is a parasite that attacks red blood cells. There are three ways Babesia spreads: 1) Through the bite of the blacklegged tick (or deer tick, Ixodes scapularis—the same tick that carries Lyme/B. burgdorferi); 2) Through blood transfusions with contaminated donated blood; 3) From mother to baby during pregnancy or childbirth.

A nymphal stage Ixodes scapularis tick (approximately the size of a poppy seed) is shown here on the back of a penny. Credit: G. Hickling, University of Tennessee.
2. The tick that carries Babesia is most likely to infect humans when it’s in its nymphal stage. During this stage, the tick is about the size of a poppy seed. (Maybe this is one reason why Babesia cases are on the rise among older people–they probably have trouble spotting ticks that small!)
3. Many people who have a Babesia infection don’t show any symptoms. When they do show symptoms, they can include fever, chills, sweats, headache, body aches, loss of appetite, nausea, and fatigue. Some develop hemolytic anemia, which causes jaundice and dark urine.
4. Babesia can be deadly if it goes untreated. Here are some possible complications: low and unstable blood pressure; altered mental status; severe hemolytic anemia (hemolysis); very low platelet count (thrombocytopenia); disseminated intravascular coagulation (also known as “DIC” or consumptive coagulopathy), which can lead to blood clots and bleeding; and malfunction of vital organs (such as the kidneys, liver, lungs, and heart).
5. There are two main treatment options for Babesia: a combination of Mepron and Zithromax OR a combination of Clindamycin and Quinine. Children and women who are pregnant should probably not be treated with Mepron.To read more about treatment, go to the Babesia fact sheet.
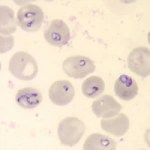
6. Babesia is sometimes confused with Malaria because they look similar under a microscope and can have similar symptoms. To avoid confusion, doctors should order multiple types of tests for Babesia if patients show symptoms. To read more about available tests, see the fact sheet.
- Babesia parasites in red blood cells on a stained blood smear. (CDC Photo: DPDx). Via CDC.gov.
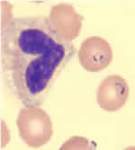
- Blood smear stained with Giemsa, showing a white blood cell (on left side) and several red blood cells, two of which are infected with Plasmodium falciparum (Malaria) (on right side). Image via CDC.gov.
7. There are 4 identified species of Babesia that infect humans: Babesia microti, B. divergens, B. duncani (WA-1), and MO-1 (unnamed strain). Antibody tests for Babesia are species specific, so if you have B. microti and you are tested for B. duncani, the test will come back negative. This means that patients need to undergo multiple blood tests!
8. Even though Babesia infection is known to be transmitted through blood transfusion (As of Sept. 2011, the CDC has identified 159 cases, and at least 12 of those people have died.), donated blood is not tested for Babesia! Donors are asked to fill out a questionnaire asking whether they have Babesia (not whether they’ve had tick bites or Babesia-like symptoms). In other words, we are relying on patient self-reporting to screen the blood supply for this parasite! (Why they don’t screen out all people who’ve had tick bites is beyond me.) The CDC’s response as to whether they will implement testing of donated blood for Babesia in the future: Maybe. They say they are going to “Monitor reports of tick-borne infection to determine if the disease is spreading to other parts of the country and to identify emerging strains of Babesia that may cause human disease.” In other words, they’re going to wait to see how bad it gets before they do anything about the blood supply. Some organizations like the Rhode Island Blood Center have begun screening blood for Babesia using an experimental test, but this is not mandated by CDC policy.
This might prompt you to ask: What are my local health department, hospitals, and blood donation organizations doing about Babesia in the blood supply?
Have questions or something to add about Babesia? Drop me a comment.
Related articles
- Well, Babs, you’re trickier than I thought (thetickthatbitme.com)
What Is Prophylaxis, and Does It Work on Tick Bites? 04/24/2012
Posted by thetickthatbitme in Peer-Reviewed, Tick-Lit, Treatment.Tags: Borrelia burgdorferi, Borrelia hermsii, Borrelia persica, CDC, doxycycline, health, Israel, Lyme Disease, medicine, NEJM, prevention, prophylaxis, research, TBRF, tick bite, treatment
3 comments
Today is Tuesday, and I’ve made an executive decision that from now on, every Tuesday I will be covering peer-reviewed research related to tick-borne infections. We in academia call this a “review of the literature,” even though it’s not what normal people think of as literature–no Shakespeare, just dry prose littered with scientific jargon–which is why most people don’t want to read it. Lucky for you, I am a super-nerd and enjoy this kind of reading, at least when it’s about TBIDs (tick-borne infectious diseases). I’ve even come up with an affectionate name for it: “tick-lit”. So every Tuesday from here on out will be Tick-Lit Tuesday, the day on which I read the literature so you don’t have to. Enjoy!
Today’s question: Does prophylaxis work for tick bites?
While a lot of patients with tick-borne infections don’t remember a tick or a tick bite (which is why it takes so long to get diagnosed), there are also people who do notice being bitten and go to a doctor right away because they are concerned about TBIDs. So what happens to these patients?
I’ve heard stories from patients with TBIDs, particularly patients with Borrelia burgdorferi (Lyme) and Borrelia hermsii (Tick-borne Relapsing Fever), about how when they went to a doctor within 48 hours of being bitten, they were told “Oh, we don’t have Lyme in this state, so you don’t have to worry.” Following this logic, ticks carrying Borrelia burgdorferi must be so smart that 1) they know which bacteria they are carrying; 2) they know which state they are in; and 3) they have the decency to respect state lines. I can really imagine a deer tick saying, “Oh, no, I can’t go over there. I’m a California tick. They don’t let dirty ticks like me out of California.” I suppose some doctors imagine that there is some kind of tick parole system that keeps them from traveling anywhere where the CDC and state health departments have not documented them to exist.
Some of these delusional doctors probably can’t be reasoned with, but what about doctors who want to do the right thing? What should they do when a patient comes to them within 48 hours of a tick bite?
Let’s take a look at the research.
One of my favorite tick-lit studies is one that was published in the New England Journal of Medicine way back in July 2006. The study took place in Israel, where Ornithodoros tholozani ticks infect people with a bacterium called Borrelia persica. Borrelia persica, like Borrelia hermsii, causes Tick Borne Relapsing Fever (TBRF). You can think of Borrelia persica as B. hermsii‘s brother. The researchers wanted to find out whether prophylaxing soldiers (giving them antibiotics right away) who had recently been bitten by ticks would prevent the infection from spreading and causing the symptoms of TBRF.
Here’s how they did it (Methods). They studied 93 healthy soldiers with suspected tick bites. Some of these people had evidence of a tick bite (like a rash) and others didn’t, but had been in the same places that the people with bites had, so they had the same risk of exposure. They randomly picked half of the soldiers who would receive antibiotics (Doxycycline for 5 days), and the other half would receive a placebo (which means they would think that they were taking antibiotics, but they were really taking a sugar pill). The study was double-blind, which means that neither the soldiers nor the researchers knew which patients were given the real antibiotics at the time of the study. This makes the study more credible.
Here’s what happened (Results):
All 10 cases of TBRF identified by a positive blood smear were in the placebo group of subjects with signs of a tick bite (P<0.001). These findings suggested a 100 percent efficacy of preemptive treatment (95 percent confidence interval, 46 to 100 percent). PCR for the borrelia glpQ gene was negative at baseline for all subjects and subsequently positive in all subjects with fever and a positive blood smear. Seroconversion was detected in eight of nine cases of TBRF. PCR and serum samples were negative for all of the other subjects tested. No major treatment-associated adverse effects were identified.
In English, this means that 10 of the 46 people who did not get treated with antibiotics got sick with TBRF, and their blood tests showed that they were making antibodies to Borrelia persica. (Their PCR test (a DNA test) was also positive for the borrelia gene.) However, none of the 47 people who were treated with antibiotics developed any symptoms of TBRF. When their blood was tested, it was negative for antibodies to Borrelia persica and their PCR was negative for the borrelia gene. That means that prophylaxing with Doxycycline prevented 100% of cases of TBRF (Borrelia perica infection).
- Doxycycline Structure. Image via Wikipedia.
- Doxycycline 3D structure. Image via Wikipedia.
Now you may say to yourself, “Oh, that’s only one study. The sample size was fairly small, and it’s not necessarily generalizable to all Borrelia infections.” At least, that’s what I imagined you (or your skeptical primary doctor) saying as I was rooting around on PubMed. Then I dug up this study from *gasp* 2001: “Prophylaxis with single-dose doxycycline for the prevention of Lyme disease after an Ixodes scapularis tick bite” (!!!)
The 2001 study was conducted in an area of New York with a high incidence of Borrelia burgdorferi (Lyme) infection. Like the Israeli study, it was also a randomized, double-blind, placebo-controlled trial, but unlike the Israeli study, they only gave patients a single dose of doxycycline. The results? One out of the 235 people treated with doxycycline got Erythema migrans, the bull’s-eye rash that indicates a Borrelia burgdorferi infection. In the placebo group (people who didn’t get antibiotics) 8 out of 235 developed the rash and tested positive for infection. Their conclusion: a single dose of doxycycline can prevent Lyme if given within 72 hours of the tick bite.
If these two studies are not convincing or current enough, the doctors from the Israeli Medical Corps published another study in 2010. First, they inform us that “Since 2004, the Israel Defence Forces (IDF) has mandated the prophylaxis of tick-bitten subjects with a five-day doxycycline course.” (That has me thinking the Israelis are pretty smart.) Just to make sure they were doing the right thing, in this study, they decided to analyze all the tick bite and TBRF cases in their records from 2004-2007.
Here’s what they say:
Of those screened, 128 (15.7%) had tick-bite and were intended for prophylaxis, of which four TBRF cases occurred-3.13% attack rate compared with an expected rate of 38.4% in these bitten individuals without prophylaxis (RR = 0.08, number needed to treat = 3). In all cases in which screening and prophylaxis were provided within 48 h of tick bite, complete prevention of TBRF was achieved. No cases of Jarisch-Herxheimer reaction (JHR) was recorded.
What does that mean? Only 4 of the 128 people who were treated with doxycycline developed TBRF, a rate of 3.13%. The expected attack rate was more than 10 times that, 38 percent, so without the doxycycline policy, it would likely have been 48 people with TBRF instead of 4. One more thing. There was a reason those four people got sick: they were given the doxycycline later than 48 hours after being bitten!
The Big Picture
How does this research affect you as a patient who has been bitten by a tick and contracted an infection or as a patient who could potentially be bitten by a tick in the future?
The research shows us that, if treated within 48 hours with 5 days of Doxycycline, most–if not all–cases of Borrelia infection and resulting symptoms can be prevented. If you could get an appointment with an infectious disease specialist who recognizes this fact within 48 hours of being bitten, you could probably avoid a lot of potential suffering. The problem is that to see a specialist, you usually need to be referred by your primary care doctor. Some of us can’t even get an appointment to see our primary care doctors within 48 hours, and some of the primary care doctors don’t even know how to spell Borrelia (no offense to primary care doctors who can spell it), let alone diagnose it with a simple blood test. And most of them certainly don’t know that the best thing to do would be to prophylax you with doxycycline.
Let’s put the numbers in perspective. In 2010, the CDC reported over 20,000 confirmed cases of Lyme (Borrelia burgdorferi) and an additional 10,000 probable cases. The CDC’s number of cases (which I believe, as with burgdorferi, are severely underreported) for 1990-2011 for Borrelia hermsii (TBRF) is 483. If 35% of those Borrelia cases had been prevented with prophylaxis, that would mean 10,669 fewer sick people.
So what can you do? Here’s a list of my suggestions:
- If you’ve been diagnosed with a tick-borne illness, make sure that every one of your doctors knows it, even the ones you don’t like and the ones you don’t go to very often. All doctors, not just infectious disease doctors, need to be aware of how prevalent these infections are.
- If you are bitten by a tick, insist that your primary care doctor prophylax you with doxycycline for five days. You can even print out these PubMed article abstracts and bring them to your appointment. Many doctors can be reasoned with, and if they won’t listen to you, sometimes they’ll listen to the New England Journal of Medicine.
- If you are bitten by a tick, try your best to save the little beast. You can store it in an old prescription bottle or a jar. (Labs like Quest Diagnostics also distribute collection containers to some doctors’ offices.) Inform your doctor that you are brining the tick to your appointment and you want to have it tested. Having ticks tested helps with more accurate CDC reporting about which areas have infected ticks.
- Getting the tick tested doesn’t mean that you don’t need to get tested. The tick testing takes longer than the people testing. On the off-chance that prophylaxis doesn’t work for you, you’ll need to get more treatment if you test positive.
- As always, the best way not to get a tick bite is not to be in areas where ticks live and not to be around animals that carry ticks. Follow tick-exposure prevention best practices. This includes keeping your home and yard free of mice and rats (on which the hermsii-carrying ticks feed) as well as deer (on which the burgdorferi-carying ticks feed).
That’s all for Tick-Lit Tuesday. Stay informed and stay well!