Four (surprising) places ticks hang out 04/30/2012
Posted by thetickthatbitme in Media, TBI Facts.Tags: Borrelia, Grizzly Peak, health, Lyme, mice, Permethrin, prevention, tick, Tilden Regional Park, yard
4 comments
Most people think you have to be hiking around in the woods to pick up a tick. In reality, ticks are a lot closer than you think. Here are four (possibly surprising) places where ticks hang out:
1. In your un-mown lawn. Ticks like to hide in vegetation to keep from drying out. Vegetation includes tall grasses, so don’t get lazy on the lawn upkeep!
2. In piles of fallen leaves. Yes, leaves are fun to jump in, and yes, the crunchy sound they make when you walk over them is lovely, but you (or your pet) could also be picking up ticks from leaf litter, so rake ’em up!
3. Anywhere mice or other rodents live. This includes wood piles, rock walls, crawl spaces, ground covers, abandoned vehicles, garbage, bushes, and palm trees. Mice also like to eat fallen fruit, so if you have fruit trees, be sure to dispose of any fruit that falls. If you have mice or rats in your home, chances are you have ticks, too. Here’s a more detailed list of mouse hiding places and what you can do to keep them away from your yard and house.
4. On and underneath wooden picnic tables and benches. To me, this is the creepiest one, because I’ve been to countless kids’ birthdays and neighborhood get-togethers in the park, and the last thing on my mind was tick exposure. If you don’t believe me when I say the risk is real, here’s an article abstract for a study conducted by Kerry Padgett and Denise Bonilla from the California Department of Public Health.
They collected ticks (some of which tested positive for Borrelia) from various areas in Berkeley’s Tilden Regional Park and found as many on wood surfaces as in leaf litter. If you’re planning on a day in the park, I recommend long pants and repellent with Permethrin.
If you’re spending time outdoors, it’s a good idea to check yourself for ticks as soon as you come inside. The University of Rhode Island’s Tick Encounter Resource Center has a great multimedia tool, the Tick Bite Locator, which suggests common places to check for ticks. They also have images of a variety of disease-carrying ticks (although the soft-bodied ones are missing) at different life stages.
Got a dog and not sure how to check him/her for ticks? WordPress blog After Gadget has a detailed explanation of how to do a thorough tick-check.
Be careful out there, everyone!
Related articles
Omelet you in on these yummy high-choline recipes 04/29/2012
Posted by thetickthatbitme in Choline Diet, Whole Person.Tags: breakfast, choline, diet, Food, leftovers, mushroom, omelet, recipe, Smoked salmon, Spinach
2 comments
In my family, omelets are somewhat of a sacred tradition. My dad was the omelet-master when I was growing up, and whenever we had weekend company, he’d make each guest and family member his or her own made-to-order omelet. By the time I was in high school, I’d picked up his technique and was making omelets for all my friends after school. Little did I know back then what a great source of the B vitamin choline omelets can be! (For more on choline, see the Choline Diet page.)The best thing about omelets besides the choline factor is the infinite possibilities–there are no rules about what cannot go in an omelet. Here are some of my favorites.
Smoked Salmon, Spinach, and Avocado Omelet
I love smoked salmon, and I’m always looking for new ways to cook with it (aside from just eating it on a bagel with cream cheese–yum). Check out this salmon omelet recipe from cuisineaustralia.com.
Choline Count: eggs (2) 200 mg + salmon (3 oz) 80 mg + spinach (2 oz) 11 mg + avocado (1) 19 mg = 300 mg of choline!
Mushroom, Spinach, and Feta Omelet
What do I like almost as much as smoked salmon? Crumbly cheeses! Feta and spinach are always delicious together, why not put them in an omelet? Add shiitake mushrooms for a bonus 66 mg of choline! Check out this recipe on closetcooking.com.
http://www.closetcooking.com/2008/03/mushroom-spinach-and-feta-omelet.html
Choline count: eggs (3) 300 mg + shiitake mushrooms (4 oz) 66 mg + spinach (2 oz) 11 mg + feta cheese (1 oz) 4 mg = 381 mg choline!
Leftover Stir-fry Omelet
This was my go-to omelet when I was a college student and rarely went grocery shopping or planned meals. I always seemed to have leftover Chinese food in my fridge, so I devised this omelet to make leftovers into breakfast. I usually use two eggs per person with a little milk. If you’ve got the jumbo eggs, you can get away with using one and use a little more milk (1 oz of skim milk has 5 mg of choline!). I whisk up the eggs and the milk in a bowl, then pour them into my omelet pan (yes, they make a size of frying pan that’s just for omelets). Meanwhile, I heat up the leftover stir-fry in a separate pan. Once that’s heated through and the egg mixture has set in the pan, I spoon some stir-fry onto one side. After a few minutes, the other side will be ready to fold over.
If you want to make a healthy stir-fry at home to use for your leftovers, you can try this recipe for Orange Ginger Beef Stir-fry from mccormick.com.
Choline count: eggs (2) 200 mg + beef sirloin (1/4 lb) 96 mg + broccoli (1/2 cup) 31 mg = 327 mg choline!
Hope you enjoyed this week’s high-choline recipes. Eggspect (sorry, I promise I’ll try to stop) to see more next Sunday!
Have a high-choline recipe (and mouth-watering photos) you’d like to showcase on this blog? E-mail thetickthatbitme AT gmail DOT com.
Related articles
Parasites in the blood supply, and 7 other things you need to know about Babesia 04/27/2012
Posted by thetickthatbitme in TBI Facts.Tags: Babesia, Blood donation, Blood transfusion, health, Malaria, medicine, Mepron, parasite, pregnancy, Rhode Island Blood Center, tick bite
6 comments
The fact sheet for Babesia is up today. Here are a few (disturbing) highlights:
1. Babesia is a parasite that attacks red blood cells. There are three ways Babesia spreads: 1) Through the bite of the blacklegged tick (or deer tick, Ixodes scapularis—the same tick that carries Lyme/B. burgdorferi); 2) Through blood transfusions with contaminated donated blood; 3) From mother to baby during pregnancy or childbirth.

A nymphal stage Ixodes scapularis tick (approximately the size of a poppy seed) is shown here on the back of a penny. Credit: G. Hickling, University of Tennessee.
2. The tick that carries Babesia is most likely to infect humans when it’s in its nymphal stage. During this stage, the tick is about the size of a poppy seed. (Maybe this is one reason why Babesia cases are on the rise among older people–they probably have trouble spotting ticks that small!)
3. Many people who have a Babesia infection don’t show any symptoms. When they do show symptoms, they can include fever, chills, sweats, headache, body aches, loss of appetite, nausea, and fatigue. Some develop hemolytic anemia, which causes jaundice and dark urine.
4. Babesia can be deadly if it goes untreated. Here are some possible complications: low and unstable blood pressure; altered mental status; severe hemolytic anemia (hemolysis); very low platelet count (thrombocytopenia); disseminated intravascular coagulation (also known as “DIC” or consumptive coagulopathy), which can lead to blood clots and bleeding; and malfunction of vital organs (such as the kidneys, liver, lungs, and heart).
5. There are two main treatment options for Babesia: a combination of Mepron and Zithromax OR a combination of Clindamycin and Quinine. Children and women who are pregnant should probably not be treated with Mepron.To read more about treatment, go to the Babesia fact sheet.
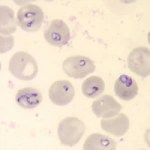
6. Babesia is sometimes confused with Malaria because they look similar under a microscope and can have similar symptoms. To avoid confusion, doctors should order multiple types of tests for Babesia if patients show symptoms. To read more about available tests, see the fact sheet.
- Babesia parasites in red blood cells on a stained blood smear. (CDC Photo: DPDx). Via CDC.gov.
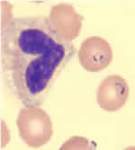
- Blood smear stained with Giemsa, showing a white blood cell (on left side) and several red blood cells, two of which are infected with Plasmodium falciparum (Malaria) (on right side). Image via CDC.gov.
7. There are 4 identified species of Babesia that infect humans: Babesia microti, B. divergens, B. duncani (WA-1), and MO-1 (unnamed strain). Antibody tests for Babesia are species specific, so if you have B. microti and you are tested for B. duncani, the test will come back negative. This means that patients need to undergo multiple blood tests!
8. Even though Babesia infection is known to be transmitted through blood transfusion (As of Sept. 2011, the CDC has identified 159 cases, and at least 12 of those people have died.), donated blood is not tested for Babesia! Donors are asked to fill out a questionnaire asking whether they have Babesia (not whether they’ve had tick bites or Babesia-like symptoms). In other words, we are relying on patient self-reporting to screen the blood supply for this parasite! (Why they don’t screen out all people who’ve had tick bites is beyond me.) The CDC’s response as to whether they will implement testing of donated blood for Babesia in the future: Maybe. They say they are going to “Monitor reports of tick-borne infection to determine if the disease is spreading to other parts of the country and to identify emerging strains of Babesia that may cause human disease.” In other words, they’re going to wait to see how bad it gets before they do anything about the blood supply. Some organizations like the Rhode Island Blood Center have begun screening blood for Babesia using an experimental test, but this is not mandated by CDC policy.
This might prompt you to ask: What are my local health department, hospitals, and blood donation organizations doing about Babesia in the blood supply?
Have questions or something to add about Babesia? Drop me a comment.
Related articles
- Well, Babs, you’re trickier than I thought (thetickthatbitme.com)
04/26/2012
Posted by thetickthatbitme in Reblogs.Tags: Letters from the Earth: Uncensored Writings (Perennial Classics), Literature, Mark Twain, microbes, nature
3 comments
Viral Pandas, a very interesting blog about the human-animal-internet connection, has a great post up today with an excerpt from Mark Twain’s “Letters from the Earth” concerning microbes and the story of Noah and the ark.
We’ve been considering the romanticised view of nature that is often portrayed online – dramatic skylines, beaming sunsets, perfectly sculpted silhouettes, and animals as well as humans placed majestically in the centre, airbrushed and beautified. Worms, bugs, and mites do not seem to exist often in this cyborg world; rarely acknowledged, spoken of, shared or liked.
We appreciate beauty, we understand.
But still, we were quite taken with this eloquent quote from Mark Twain’s ‘Letters from the Earth’; a poetic, beautifully written description of the very thing that usually makes us squirm.
Perhaps it still does, just a little, but we’ve taken it as inspiration for the opposite of our domesticated head – the ‘Wild Man’ (coming soon!).
Mark Twain
“Noah and his family were saved — if that could be called an advantage. I throw in the if for the reason that there has never been an intelligent person…
View original post 308 more words
Eight things you need to know about Anaplasmosis 04/25/2012
Posted by thetickthatbitme in Diagnosis, TBI Facts.Tags: Anaplasma phagocytophilum, Anaplasmosis, Borrelia burgdorferi, doxycycline, health, labs, Lyme Disease, medicine, Rocky Mountain Spotted Fever, tick, treatment
5 comments
A new fact sheet is up today for Anaplasmosis, otherwise known as Anaplasma phagocytophilum infection. Try saying that three times fast. This is one of the two TBIDs I’ve been unlucky enough to have, but I had never heard of it before my lab results came back with a positive antibody test for it. By the end of this post, you’ll know eight things you didn’t know before about Anaplasmosis.

A microcolony of A. phagocytophylum visible in a granulocyte (white blood cell) on a peripheral blood smear. Image via CDC.gov.
1. Anaplasmosis is spread by the same ticks that spread Borrelia burgdorferi (Lyme Disease). This means that people with Lyme can have a coinfection with Anaplasmosis (and some of them don’t know it).
2. The symptoms of an Anaplasma phagocytophilum infection are: fever, headache, muscle pain, malaise, chills, nausea / abdominal pain, cough, and confusion. Some people get all the symptoms; other people only get a few.
3. If you show symptoms of Anaplasmosis, your doctor shouldn’t wait for lab results to come back to begin treating you. The CDC recommends beginning treatment right away.
4. If you’ve been infected with Anaplasma phagocytophilum and you get tested within the first 7-10 days you are sick, the test might come back negative. This doesn’t mean you don’t have Anaplasmosis, and you’ll need to be tested again later.
5. The best way to treat Anaplasmosis is with the antibiotic Doxycycline. According to the CDC, other antibiotics should not be substituted because they increase the risk of fatality. If your doctor insists on treating your Anaplasmosis with something other than Doxycycline, it’s probably time to get a new doctor. For people with severe allergies to Doxycycline or for women who are pregnant, the drug Rifampin can be used to treat Anaplasmosis.
6. Anaplasmosis can be confused with other TBIDs in the rickettsia family like Rocky Mountain Spotted Fever (RMSF) and ehrlichiosis. These infections are also commonly treated with Doxycycline.
7. The number of cases of Anaplasmosis reported to the CDC has increased steadily since 1996. You can attribute this to climate change or not, but the trend suggests that this disease will be an increasingly more common problem in the future.
8. More than half of Anaplasmosis cases are reported in the spring and summer months. This is a no-brainer, since this is when tick populations thrive. To avoid infection, take steps to avoid tick exposure for both you and your pets.
What Is Prophylaxis, and Does It Work on Tick Bites? 04/24/2012
Posted by thetickthatbitme in Peer-Reviewed, Tick-Lit, Treatment.Tags: Borrelia burgdorferi, Borrelia hermsii, Borrelia persica, CDC, doxycycline, health, Israel, Lyme Disease, medicine, NEJM, prevention, prophylaxis, research, TBRF, tick bite, treatment
3 comments
Today is Tuesday, and I’ve made an executive decision that from now on, every Tuesday I will be covering peer-reviewed research related to tick-borne infections. We in academia call this a “review of the literature,” even though it’s not what normal people think of as literature–no Shakespeare, just dry prose littered with scientific jargon–which is why most people don’t want to read it. Lucky for you, I am a super-nerd and enjoy this kind of reading, at least when it’s about TBIDs (tick-borne infectious diseases). I’ve even come up with an affectionate name for it: “tick-lit”. So every Tuesday from here on out will be Tick-Lit Tuesday, the day on which I read the literature so you don’t have to. Enjoy!
Today’s question: Does prophylaxis work for tick bites?
While a lot of patients with tick-borne infections don’t remember a tick or a tick bite (which is why it takes so long to get diagnosed), there are also people who do notice being bitten and go to a doctor right away because they are concerned about TBIDs. So what happens to these patients?
I’ve heard stories from patients with TBIDs, particularly patients with Borrelia burgdorferi (Lyme) and Borrelia hermsii (Tick-borne Relapsing Fever), about how when they went to a doctor within 48 hours of being bitten, they were told “Oh, we don’t have Lyme in this state, so you don’t have to worry.” Following this logic, ticks carrying Borrelia burgdorferi must be so smart that 1) they know which bacteria they are carrying; 2) they know which state they are in; and 3) they have the decency to respect state lines. I can really imagine a deer tick saying, “Oh, no, I can’t go over there. I’m a California tick. They don’t let dirty ticks like me out of California.” I suppose some doctors imagine that there is some kind of tick parole system that keeps them from traveling anywhere where the CDC and state health departments have not documented them to exist.
Some of these delusional doctors probably can’t be reasoned with, but what about doctors who want to do the right thing? What should they do when a patient comes to them within 48 hours of a tick bite?
Let’s take a look at the research.
One of my favorite tick-lit studies is one that was published in the New England Journal of Medicine way back in July 2006. The study took place in Israel, where Ornithodoros tholozani ticks infect people with a bacterium called Borrelia persica. Borrelia persica, like Borrelia hermsii, causes Tick Borne Relapsing Fever (TBRF). You can think of Borrelia persica as B. hermsii‘s brother. The researchers wanted to find out whether prophylaxing soldiers (giving them antibiotics right away) who had recently been bitten by ticks would prevent the infection from spreading and causing the symptoms of TBRF.
Here’s how they did it (Methods). They studied 93 healthy soldiers with suspected tick bites. Some of these people had evidence of a tick bite (like a rash) and others didn’t, but had been in the same places that the people with bites had, so they had the same risk of exposure. They randomly picked half of the soldiers who would receive antibiotics (Doxycycline for 5 days), and the other half would receive a placebo (which means they would think that they were taking antibiotics, but they were really taking a sugar pill). The study was double-blind, which means that neither the soldiers nor the researchers knew which patients were given the real antibiotics at the time of the study. This makes the study more credible.
Here’s what happened (Results):
All 10 cases of TBRF identified by a positive blood smear were in the placebo group of subjects with signs of a tick bite (P<0.001). These findings suggested a 100 percent efficacy of preemptive treatment (95 percent confidence interval, 46 to 100 percent). PCR for the borrelia glpQ gene was negative at baseline for all subjects and subsequently positive in all subjects with fever and a positive blood smear. Seroconversion was detected in eight of nine cases of TBRF. PCR and serum samples were negative for all of the other subjects tested. No major treatment-associated adverse effects were identified.
In English, this means that 10 of the 46 people who did not get treated with antibiotics got sick with TBRF, and their blood tests showed that they were making antibodies to Borrelia persica. (Their PCR test (a DNA test) was also positive for the borrelia gene.) However, none of the 47 people who were treated with antibiotics developed any symptoms of TBRF. When their blood was tested, it was negative for antibodies to Borrelia persica and their PCR was negative for the borrelia gene. That means that prophylaxing with Doxycycline prevented 100% of cases of TBRF (Borrelia perica infection).
- Doxycycline Structure. Image via Wikipedia.
- Doxycycline 3D structure. Image via Wikipedia.
Now you may say to yourself, “Oh, that’s only one study. The sample size was fairly small, and it’s not necessarily generalizable to all Borrelia infections.” At least, that’s what I imagined you (or your skeptical primary doctor) saying as I was rooting around on PubMed. Then I dug up this study from *gasp* 2001: “Prophylaxis with single-dose doxycycline for the prevention of Lyme disease after an Ixodes scapularis tick bite” (!!!)
The 2001 study was conducted in an area of New York with a high incidence of Borrelia burgdorferi (Lyme) infection. Like the Israeli study, it was also a randomized, double-blind, placebo-controlled trial, but unlike the Israeli study, they only gave patients a single dose of doxycycline. The results? One out of the 235 people treated with doxycycline got Erythema migrans, the bull’s-eye rash that indicates a Borrelia burgdorferi infection. In the placebo group (people who didn’t get antibiotics) 8 out of 235 developed the rash and tested positive for infection. Their conclusion: a single dose of doxycycline can prevent Lyme if given within 72 hours of the tick bite.
If these two studies are not convincing or current enough, the doctors from the Israeli Medical Corps published another study in 2010. First, they inform us that “Since 2004, the Israel Defence Forces (IDF) has mandated the prophylaxis of tick-bitten subjects with a five-day doxycycline course.” (That has me thinking the Israelis are pretty smart.) Just to make sure they were doing the right thing, in this study, they decided to analyze all the tick bite and TBRF cases in their records from 2004-2007.
Here’s what they say:
Of those screened, 128 (15.7%) had tick-bite and were intended for prophylaxis, of which four TBRF cases occurred-3.13% attack rate compared with an expected rate of 38.4% in these bitten individuals without prophylaxis (RR = 0.08, number needed to treat = 3). In all cases in which screening and prophylaxis were provided within 48 h of tick bite, complete prevention of TBRF was achieved. No cases of Jarisch-Herxheimer reaction (JHR) was recorded.
What does that mean? Only 4 of the 128 people who were treated with doxycycline developed TBRF, a rate of 3.13%. The expected attack rate was more than 10 times that, 38 percent, so without the doxycycline policy, it would likely have been 48 people with TBRF instead of 4. One more thing. There was a reason those four people got sick: they were given the doxycycline later than 48 hours after being bitten!
The Big Picture
How does this research affect you as a patient who has been bitten by a tick and contracted an infection or as a patient who could potentially be bitten by a tick in the future?
The research shows us that, if treated within 48 hours with 5 days of Doxycycline, most–if not all–cases of Borrelia infection and resulting symptoms can be prevented. If you could get an appointment with an infectious disease specialist who recognizes this fact within 48 hours of being bitten, you could probably avoid a lot of potential suffering. The problem is that to see a specialist, you usually need to be referred by your primary care doctor. Some of us can’t even get an appointment to see our primary care doctors within 48 hours, and some of the primary care doctors don’t even know how to spell Borrelia (no offense to primary care doctors who can spell it), let alone diagnose it with a simple blood test. And most of them certainly don’t know that the best thing to do would be to prophylax you with doxycycline.
Let’s put the numbers in perspective. In 2010, the CDC reported over 20,000 confirmed cases of Lyme (Borrelia burgdorferi) and an additional 10,000 probable cases. The CDC’s number of cases (which I believe, as with burgdorferi, are severely underreported) for 1990-2011 for Borrelia hermsii (TBRF) is 483. If 35% of those Borrelia cases had been prevented with prophylaxis, that would mean 10,669 fewer sick people.
So what can you do? Here’s a list of my suggestions:
- If you’ve been diagnosed with a tick-borne illness, make sure that every one of your doctors knows it, even the ones you don’t like and the ones you don’t go to very often. All doctors, not just infectious disease doctors, need to be aware of how prevalent these infections are.
- If you are bitten by a tick, insist that your primary care doctor prophylax you with doxycycline for five days. You can even print out these PubMed article abstracts and bring them to your appointment. Many doctors can be reasoned with, and if they won’t listen to you, sometimes they’ll listen to the New England Journal of Medicine.
- If you are bitten by a tick, try your best to save the little beast. You can store it in an old prescription bottle or a jar. (Labs like Quest Diagnostics also distribute collection containers to some doctors’ offices.) Inform your doctor that you are brining the tick to your appointment and you want to have it tested. Having ticks tested helps with more accurate CDC reporting about which areas have infected ticks.
- Getting the tick tested doesn’t mean that you don’t need to get tested. The tick testing takes longer than the people testing. On the off-chance that prophylaxis doesn’t work for you, you’ll need to get more treatment if you test positive.
- As always, the best way not to get a tick bite is not to be in areas where ticks live and not to be around animals that carry ticks. Follow tick-exposure prevention best practices. This includes keeping your home and yard free of mice and rats (on which the hermsii-carrying ticks feed) as well as deer (on which the burgdorferi-carying ticks feed).
That’s all for Tick-Lit Tuesday. Stay informed and stay well!
Pink Deer and TBID Prevention 04/23/2012
Posted by thetickthatbitme in Media.Tags: deer, Fairfax County, Lyme, pink, prevention, tick, tick-borne illness, Virginia, Washington Post
2 comments
We all know (I hope) that an ever-increasing deer population means an ever-increasing tick population. We may not be able to stop the deer from multiplying (although I hear some are trying with bowhunting), but can we stop the ticks?

Fairfax Wildlife Biologist Vicky Monroe displays the day-glo pink pesticide that will show up on deer and any other animal who visits the county’s new feeders. Image via The Washington Post.
A March 26 article in the Washington Post describes a study the Fairfax County (Virginia) Wildlife Biologist’s Office (in collaboration with the county’s Disease Carrying Insects Program) is undertaking in which deer are attracted to feeders with corn and simultaneously treated with permethrin, a tick-killing pesticide. The twist? The pesticide has been dyed pink to allow for easier tracking of the deer. Fairfax County residents can expect to see not only pink deer, but also squirrels, raccoons, birds, and any other fauna that stop by for a snack.
How will this aid research on and prevention of tick-borne illness? Washington Post’s Tom Jackman explains:
On a couple of days every other month for the next three years, the pink deer will be harvested (or “killed,” in non-wildlife biologist terms) and autopsied. Deer organs will be tested and the remaining ticks will be sent to a lab for detailed analysis
Thus, the pink deer study will help the Fairfax County Wildlife Biologist’s office determine how effective the feeder-application of the pesticide is in killing disease-carrying ticks on the deer.
The study is costing the Fairfax County Health Department $380,000. For those in the county who have been affected by tick-borne infectious diseases (TBIDs), I’m sure this is not too high a price.
Would you support programs like this in your community? What is your county doing to control the vector population and prevent TBIDs?
Eat Your Eggs, Benedict! 04/22/2012
Posted by thetickthatbitme in Choline Diet, Whole Person.Tags: Anaplasmosis, benedict, Borrelia burgdorferi, Borrelia hermsii, choline, diet, eggs, HBO, inflammation, Lyme, mushroom, recipe, salmon
5 comments
If you know my story, you know that when I was diagnosed with B. hermsii and Anaplasmosis, my doctor put me on a high-choline diet. Why choline, you ask? Choline is a B vitamin that aids in the transmission of nerve impulses from the brain through the central nervous system–this process is essential to functions like memory and muscle control. Since Borrelia like to attack the central nervous system, choline is especially important for people with (past and present) B. hermsii and B. burgdorferi infections. People who eat diets high in choline have also been shown to have lower levels of inflammation (like inflammation of the joints in Arthritis) than people who don’t. You can read more about choline here.
Enter the Benedict. It is by far my favorite egg-based dish, and I enjoy making it at home just as much as I do eating it for brunch in a fancy restaurant.
One large poached egg has 100 mg of choline, so if you eat two, you get about half of your recommended daily amount (425 mg for women, 550 mg for men). Add to that other high-choline foods like smoked salmon (129 mg), Canadian bacon (39 mg), portabella mushrooms (39 mg), spinach (35 mg), asparagus (23 mg), avocado (21 mg), and tomato (6 mg) to get your choline fix!
Here are my top five Benedicts:
1. Old Fashioned but Fried
for those mornings (or afternoons, or evenings!) when I’m feeling traditional, yet lazy
I learned this simple recipe from my mother, and it
brings back all kinds of fond childhood memories. A toasted whole-wheat English muffin, topped with pan-fried Canadian bacon and over-easy eggs (make sure they’re still a little runny, because that’s the best part). The hollandaise sauce I usually make with one of those sauce packets you can find in the grocery store (next to the gravy packets). It’s easy–you only need to add milk and butter–and, in my opinion, it tastes better than the from-scratch hollandaise recipes I’ve tried. Because of the butter and bacon, this is a slightly fattening meal, so I balance it with a side of boiled asparagus, which tastes delicious with the hollandaise sauce and adds 23 mg of choline to this meal!
Choline count: eggs 200 mg + Canadian bacon 39 mg + asparagus 23 mg = 262 mg of choline
2. Crab Benedict
for when I’m feeling crabby or rooting for the Terps
I’ve never made this one at home, but I’ve had it at Toasties Cafe, and it is delicious!
Choline count: eggs 200 mg
3. Portabello Mushroom Benedict
for the fungus-lovers amongus
If you’re looking for a meatless meal or just craving these yummy mushrooms, this is the Benedict for you. Check out Jackie Dodd’s recipe at TastyKitchen.com, which also includes spinach, tomatoes, and Sriracha for a kick!
Choline count: eggs 200 mg + portabello mushrooms 39 mg + spinach 35 mg = 274 mg of choline
4. Tomato Avocado Benedict
because I’m a California girl
My mouth was watering as I scrolled through SoupBelly.com’s deliciously illustrated recipe for this west-coast Benedict. If you want to make it even more California, use sourdough English muffins.
Choline count: eggs 200 mg + avocado 21 mg + tomato 6 mg = 227 mg of choline
5. Eggs Hemingway
for when I’m feeling literary
This one may seem a bit fishy, but I assure you it’s delicious and packed with choline. It’s also called Norwegian Benedict. Here’s a recipe at food.com that includes not only salmon but spinach, too!
Choline count: eggs 200 mg + smoked salmon 129 mg + spinach 35 mg = 364 mg of choline
Now that I’ve made myself really hungry, I’m going to go make my own Benedict. Hope you enjoy these eggcellent (sorry, I couldn’t resist) high-choline meals!
Curious about Tick-borne Infections? 04/21/2012
Posted by thetickthatbitme in TBI Facts.Tags: Borrelia burgdorferi, Borrelia hermsii, diagnosis, facts, infection, Lyme, Lyme Disease, TBI, tick-borne, treatment, ugly stepsister
2 comments
Happy Saturday, loyal readers!
I thought I’d point out that I’ve added a new section to the blog: Infection Fact Sheets. One of my goals with this blog is to give you, my readers, access to as much factual information about tick-borne infectious diseases–or TBIDs, as I like to abbreviate them–as possible.
Since you’ve stumbled upon this blog, I’m sure you’ve heard of Lyme Disease, but do you know the name of the bacterium that causes it? Are you familiar with the common and not-so-common symptoms? What about the different drugs that are used to treat this infection? Check out the fact sheet here.
And let’s not forget Borrelia hermsii, which I consider to be like Lyme’s neglected ugly stepsister. Nope, no press for Ms. B. hermsii… Take pity on her (or if not her, me, a hermsii survivor) and pay a visit to her fact sheet.
If I were truly going to put my teacher hat on and plan a lesson for you, I’d tell you to make a K-W-L chart and take notes!
Once you’re done with the Borrelia sisters, you’ll probably be hungering (or worrying?) for more TBID info. Here’s a list of what’s to come: Anaplasmosis, Babesiosis (WA-1), Ehrlichiosis, Rickettsia (Rocky Mountain Spotted Fever), and more!
“Persistent Infection With Lyme Disease” Dr Phil – YouTube 04/20/2012
Posted by thetickthatbitme in Media.Tags: azithromycin, board certification, Borrelia burgdorferi, Ceftriaxone, chronic Lyme, doctors, Dr. Phil, IV antibiotics, Lyme Disease, Lyme-literate, media, misdiagnosis, PICC line, TV
add a comment
If you missed the April 13 episode of Dr. Phil on which Lyme Disease was discussed, you can watch it on YouTube.
“Persistent Infection With Lyme Disease” Dr Phil – YouTube.
Here are my reactions:
9:24 When she says she is positive for 4 strains of Lyme, I assume that she means that 4 bands (out of 10) on her western blot were reactive (positive). The word “strain” is misleading because it makes it sound like she has 4 different infections. Lyme Disease is caused by one species of bacteria named Borrelia burgdorferi. There are, however, other bacteria in the Borrelia genus that cause Lyme-like symptoms–B. hermsii being one of them.
9:41 She has a PICC line, which is more convenient for the doctor because she doesn’t have to stick her with a needle every day, but the risk of secondary infection is much higher than getting a new IV in the hand everyday.
9:45 Five IVs a DAY?!?! WHY?
9:52 Why is she being treated with IV Zithromax and not Ceftriaxone? (Zithromax/azithromycin is what you take orally when you have Strep throat.) I guess this explains the 5 IVs per day. Maybe if they used the right drug, she could cut back to one IV per day.
10:16 That freaks me out that she’s speeding up her own drip. Only the doctor is supposed to do that! (If the drip goes too fast, you can have a nasty adverse reaction.)
11:57 I wonder which tests she got, and in what order.
14:30 Here’s Dr. Auwaerter’s CV, if you’re curious. Scroll down to the publications.
15:08 You can read the text of the monkey study Dr. Bhakta alludes to here. BTW, Dr. Bhakta’s residencies were in Respiratory Therapy and Anesthesiology. She is not board certified in California. To read more about board certification, go here.
What were your thoughts on this episode? Drop me a comment.