Six Tick Misconceptions 07/05/2012
Posted by thetickthatbitme in Diagnosis, Prevention, TBI Facts.Tags: Babesia, Borrelia, Colorado Tick Fever, health, Lyme Disease, medicine, misconception, Ornithodoros, prevention, Rickettsiosis, Rocky Mountain Spotted Fever, tick, Tick-borne disease
4 comments
I have a confession to make. I have a phobia of most creepy-crawly things–roaches, mosquitoes, spiders, and especially ticks. When I see pictures of any of these critters, my first instinct is to shield my eyes. Ick! But what I should be doing is taking notice, so that if a tick ever gets on me again, maybe I can identify that little jerk.
Today’s post is about the misconceptions that many people have about ticks. As I warn frequently, there’s a lot of misinformation about ticks and the diseases they spread in the mainstream media and on the Internet. Here are six big misconceptions.
#1: Only deer ticks transmit diseases.
Deer ticks (a.k.a. blacklegged ticks) carry a lot of pathogens, including those that cause Lyme disease, Anaplasmosis, Babesiosis, and Bartonellosis, but they’re not the only ones you need to worry about. Dog ticks (Dermacentor variabilis) and wood ticks (Dermacentor andersoni) carry Rocky Mountain spotted fever (Rickettsiosis), Tularemia, and the Colorado Tick Fever virus. The lone star tick (Ambylomma americanum) carries Ehrlichiosis and the pathogen that causes STARI; bites from this tick have also been linked to a delayed allergic reaction to red meat. Two other types of Rickettsiosis, Rickettsia parkeri and 364D Rickettsiosis can be transmitted by the Gulf Coast tick (Amblyomma maculatum) and the Pacific Coast tick (Dermacentor occidentalis), respectively. Q fever (Coxiella burnetii) can be transmitted by the brown dog tick (Rhipicephalus sanguineus), Rocky Mountain wood tick (Dermacentor andersoni), and the lone star tick (Amblyomma americanum). Last but not least, soft-bodied ticks like Ornithodoros hermsi, Ornithodoros parkeri, and Ornithodoros turicata transmit Relapsing Fever-causing species of Borrelia. These ticks can live up to ten years!
#2: Lyme disease is the most dangerous thing I can get from a tick.
Though life-threatening complications like myocarditis can occur in the later stages of Lyme disease, B. burgdorferi infection is rarely fatal in the first months of infection. Many patients survive years without being properly diagnosed and treated. By contrast, Rickettsiosis (Rocky Mountain spotted fever) can be fatal in the first 8 days of symptoms (which vary greatly from person to person and don’t always involve the spotted rash) if it goes untreated. Female tick saliva also contains a neurotoxin that can cause tick paralysis, which can be fatal if the tick is not found and removed.
#3: I can’t get sick unless the tick is attached 36-48 hours.
While the CDC claims this is true for Lyme disease, if the tick has bitten you, there’s always a chance that bacteria or a virus is already in your system. Even if the tick doesn’t infect you with bacteria or a virus, you are still at risk for tick paralysis (see #2). In the case of soft-bodied Ornithodoros ticks, which spread Relapsing Fever Borrelia, feeding may only take a few minutes, and then the tick falls off, often undetected. (You can read more about soft-bodied ticks here.)
#4: If I don’t go hiking or camping, I’m not going to get bitten by a tick.
While participation in these activities does put you at higher risk for tick exposure, ticks can hide out in plenty of other places besides the forest floor, including the leaf litter in your yard. Ticks can hitch a ride into your yard on any of the wildlife on which they feed, including deer, mice, squirrels, and birds. They can hitch a ride into your house on your dog or cat. And don’t forget other four-legged friends like horses and sheep. If you have mice in your house or attic, you probably also have ticks. To avoid exposure, you should limit your contact with leaf litter, tall grasses, wood piles, and bird feeders. When hiking, stay in the middle of trails, wear long pants tucked into your socks, and wear repellent. Avoid sleeping in cabins that may be infested with rodents (and thereby ticks). After spending time outdoors or with animals, do a thorough tick-check. (This requires getting naked.) And if you’re a fan of spelunking, know that ticks—particularly soft-bodied ones—can live in caves too.
#5: If I don’t have a rash or a fever, the tick that bit me didn’t give me a disease.
At least 20% of people infected with Borrelia burgdorferi (Lyme) don’t have the characteristic erythema chronicum migrans (bull’s-eye) rash (EM). People with other tick-borne illnesses may be asymptomatic or have other symptoms (like joint and muscle pain or fatigue) that may not directly suggest an infection. That’s why it’s important to keep track of all of your symptoms following a tick bite, and to save the tick for identification and testing. You should always make sure your doctor is aware of any tick bites or tick exposures you may have had—and be clear about what regions/countries you’ve visited and what animal exposure you’ve had.
#6: I can use soap or Vaseline to remove a tick, and afterwards I should burn it with a match.
The proper way to remove a tick is with tweezers, grabbing the tick close to the skin, and using a slow, steady motion to pull it out. Using soap or Vaseline will not help you get a better grip on the tick, and may increase the likelihood that you squeeze the tick, causing it to regurgitate bacteria and other pathogens into your skin. Once you remove the tick, you should store it in a secure container and bring it to your doctor’s office for identification and testing. If you do get sick, it will be helpful to know what kind of tick it is and what pathogens it’s carrying. Don’t destroy the evidence with a match! If for some reason you can’t save the tick (because you’re too busy spelunking), at the very least try to take a picture of it. You’ll probably need a zoom lens.
So how do I spot them?
I usually try to link to pictures of ticks instead of posting them on this site because seeing tick photos can be a bit traumatizing to those of us who have been sick with tick-borne infections. However, for the purpose of prevention education, I’ve included pictures of all the ticks mentioned in this post (that I could find) in the slideshow below. You can read about the geographic distribution of hard-bodied ticks in the U.S. here and the habitats of soft-bodied ticks here.
Related articles
Well, Babs, you’re trickier than I thought 05/01/2012
Posted by thetickthatbitme in Diagnosis, Peer-Reviewed, TBI Facts, Tick-Lit.Tags: Babesia, Blood donation, Blood transfusion, health, IFA, labs, Lyme, medicine, PCR, smear, tick
1 comment so far
Welcome to the second installment of Tick-Lit Tuesday, where I comb through PubMed so you don’t have to. Today’s topic: Babesia and Blood Transfusions. Now, I know I posted about Babesia in the blood supply just a few days ago, but an interesting study has since come to my attention (thanks, Dr. W), and the implications are a bit scary. Okay, get your popcorn and let’s begin.
The Issue:
It has been well-documented that the tick-borne protozoan parasite Babesia can be contracted through blood transfusions. Blood centers aren’t required to test donated blood for Babesia, but this may change in the future, as Babesia infections contracted through transfusions are on the rise. So if we were to test all donors for Babesia prior to donation, which tests should we rely on to detect this pesky parasite? Let’s look at the candidates.
IFA: IFA is an abbreviation for indirect fluorescent antibody test. This type of test can also be referred to as serologic (as in blood serum) testing. If you’ve had one of these tests for Babesia, it’s probably titled something like “WA1 IGG ANTIBODY IFA” (for B. duncani) or “BABESIA MICROTI ABS IGG/IGM” on your lab results. If you’ve had Babesia in the past and been treated for it, your antibody test might still read positive because your body is still making antibodies to the parasite. This is one of the reasons why most insurance companies refuse to pay for treatment for Babesia if your only positive test is the IFA. They think maybe you had a past infection that you got over, so you don’t need treatment. (The other reason they refuse to pay is that they’re jerks, to put it nicely.) I’ll talk more about why this is such a problem later in this post.

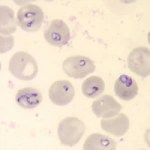
A stained blood smear on which B. microti parasites are visible in red blood cells. (CDC Photo: DPDx). Via CDC.gov.
Smear: When we talk about a smear for Babesia, we mean a Giemsa-stained thin blood smear. This test involves looking at blood samples under a microscope to see if there are any parasites hanging around. The problem with this test is that Babesia can infect fewer than 1% of your circulating red blood cells, so it could take many, many smears before any Babesia show up under the microscope. For more information about that phenomenon, read this.
PCR: This stands for polymerase chain reaction. It’s basically a DNA test that tries to identify whether a gene associated with Babesia is present in the blood. PCR has been found to be “as sensitive and specific” as blood smears for Babesia (see this study), which is not saying much, considering the tendency of Babesia to go undetected with smears.
Hmmm, for whom shall I cast my ballot, the antibody test insurance companies don’t trust, the inaccurate smear, or the inaccurate PCR? Choices, choices…
Today’s question:
Can the donated blood of someone with a negative PCR and negative blood smear still be infected with Babesia and cause Babesia infection in transfusion recipients?
(Hint: This is a leading question.)
Let’s talk about a study published in the journal Transfusion in December of 2011 called “The third described case of transfusion-transmitted Babesia duncani.”
Here’s what happened:
In May 2008, a 59 year-old California resident (I’ll call him Cal) with sickle-cell disease had some red blood cell transfusions. Cal’s only risk factor for Babesia was the transfusions; he didn’t have any tick exposure. In September of 2008, Cal was diagnosed with a Babesia duncani (WA-1) infection. The parasites were visible on a blood smear, the indirect fluorescent antibody (IFA) test was positive, and the PCR was positive for the Babesia gene. This launched a transfusion investigation in which doctors tracked down 34 of the 38 blood donors whose blood could have infected Cal with Babesia. One donor, a 67-year-old California resident (who I’ll call Don) had a B. duncani titer of 1:4096 (on the IFA test). What does a titer of 1:4096 mean? Well, if the antibody test for B. duncani is negative, the titer will be < 1:256. That means that Don’s antibody test was positive.
What the article abstract doesn’t tell you, which the full article does, is that both Don’s PCR and blood smear were negative for Babesia. How did the researchers prove definitively that Don had Babesia in his blood? They injected the blood into Mongolian gerbils, and were later able to isolate the parasite from the gerbils. Conclusion: Even though Don showed no symptoms of Babesia and both his PCR and smear were negative, his donated blood caused Babesiosis in both Cal and the gerbils.
Here’s why the study’s findings are important:
1. Clearly, blood smears and PCRs are not good indicators of whether someone is infected with Babesia. Why insurance companies think these tests need to be positive before they’ll pay for treatment is a mystery to me. There are probably a lot of people out there who’ve had positive IFAs but negative smear and/or PCR who were then not treated for Babesia because either the doctor, the insurance company, or both said they didn’t have an infection.
2. As far as the blood donation goes, if we don’t start screening out donors with positive Babesia IFAs, we’re going to continue to contaminate the blood supply with Babesia. It should be as simple as that. Been bitten by a tick? No blood donation for you. Positive IFA? No blood donation for you.
DZWSQK6QYS9G
Related articles
Parasites in the blood supply, and 7 other things you need to know about Babesia 04/27/2012
Posted by thetickthatbitme in TBI Facts.Tags: Babesia, Blood donation, Blood transfusion, health, Malaria, medicine, Mepron, parasite, pregnancy, Rhode Island Blood Center, tick bite
6 comments
The fact sheet for Babesia is up today. Here are a few (disturbing) highlights:
1. Babesia is a parasite that attacks red blood cells. There are three ways Babesia spreads: 1) Through the bite of the blacklegged tick (or deer tick, Ixodes scapularis—the same tick that carries Lyme/B. burgdorferi); 2) Through blood transfusions with contaminated donated blood; 3) From mother to baby during pregnancy or childbirth.

A nymphal stage Ixodes scapularis tick (approximately the size of a poppy seed) is shown here on the back of a penny. Credit: G. Hickling, University of Tennessee.
2. The tick that carries Babesia is most likely to infect humans when it’s in its nymphal stage. During this stage, the tick is about the size of a poppy seed. (Maybe this is one reason why Babesia cases are on the rise among older people–they probably have trouble spotting ticks that small!)
3. Many people who have a Babesia infection don’t show any symptoms. When they do show symptoms, they can include fever, chills, sweats, headache, body aches, loss of appetite, nausea, and fatigue. Some develop hemolytic anemia, which causes jaundice and dark urine.
4. Babesia can be deadly if it goes untreated. Here are some possible complications: low and unstable blood pressure; altered mental status; severe hemolytic anemia (hemolysis); very low platelet count (thrombocytopenia); disseminated intravascular coagulation (also known as “DIC” or consumptive coagulopathy), which can lead to blood clots and bleeding; and malfunction of vital organs (such as the kidneys, liver, lungs, and heart).
5. There are two main treatment options for Babesia: a combination of Mepron and Zithromax OR a combination of Clindamycin and Quinine. Children and women who are pregnant should probably not be treated with Mepron.To read more about treatment, go to the Babesia fact sheet.
6. Babesia is sometimes confused with Malaria because they look similar under a microscope and can have similar symptoms. To avoid confusion, doctors should order multiple types of tests for Babesia if patients show symptoms. To read more about available tests, see the fact sheet.
- Babesia parasites in red blood cells on a stained blood smear. (CDC Photo: DPDx). Via CDC.gov.
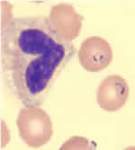
- Blood smear stained with Giemsa, showing a white blood cell (on left side) and several red blood cells, two of which are infected with Plasmodium falciparum (Malaria) (on right side). Image via CDC.gov.
7. There are 4 identified species of Babesia that infect humans: Babesia microti, B. divergens, B. duncani (WA-1), and MO-1 (unnamed strain). Antibody tests for Babesia are species specific, so if you have B. microti and you are tested for B. duncani, the test will come back negative. This means that patients need to undergo multiple blood tests!
8. Even though Babesia infection is known to be transmitted through blood transfusion (As of Sept. 2011, the CDC has identified 159 cases, and at least 12 of those people have died.), donated blood is not tested for Babesia! Donors are asked to fill out a questionnaire asking whether they have Babesia (not whether they’ve had tick bites or Babesia-like symptoms). In other words, we are relying on patient self-reporting to screen the blood supply for this parasite! (Why they don’t screen out all people who’ve had tick bites is beyond me.) The CDC’s response as to whether they will implement testing of donated blood for Babesia in the future: Maybe. They say they are going to “Monitor reports of tick-borne infection to determine if the disease is spreading to other parts of the country and to identify emerging strains of Babesia that may cause human disease.” In other words, they’re going to wait to see how bad it gets before they do anything about the blood supply. Some organizations like the Rhode Island Blood Center have begun screening blood for Babesia using an experimental test, but this is not mandated by CDC policy.
This might prompt you to ask: What are my local health department, hospitals, and blood donation organizations doing about Babesia in the blood supply?
Have questions or something to add about Babesia? Drop me a comment.
Related articles
- Well, Babs, you’re trickier than I thought (thetickthatbitme.com)